Strabismus
Strabismus is the medical term for eyes that point in different directions. Strabismus is common, affecting 2-3% of the population to some degree. When thinking about strabismus, it is useful to break it down into the simple pieces: horizontal and vertical alignment. There are 3 forms commonly seen:
- Eyes turn towards the nose (eso-deviation)
- Eyes turn towards the ears (exo-deviation)
- One eye is higher than the other (hyper-deviation)
Less commonly, vertical and horizontal deviations co-exist; there can be rotational misalignment; and the size (and direction) of the strabismus may vary depending on where the person looks. Adding to the fun, there are always “exceptions to the rule.” Experienced strabismus specialists know how to evaluate the alignment of the eyes and offer treatment options.
Notice that the plural “eyes” is used here. Even though only one eye looks to be misaligned, in fact, strabismus involves both eyes. The eyes are misaligned relative to each other.
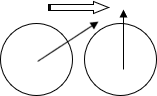
For example: someone has strabismus causing their eyes to turn 30 degrees towards the nose (eso-deviation). Let’s say their right eye is looking directly at you. This means that all 30 degrees of the turn must be taken up by the left eye. We are tempted to say, “the left eye is turned, and the right is straight” but, in fact, the eyes are turned towards each other 30 degrees. If you covered the right eye, the left eye would look directly at you and – under the cover – the right eye would turn in 30 degrees.
Esotropia: Both eyes are turning in towards the nose.
The person must use one eye to look straight ahead so both eyes will shift in that direction. Here, the left eye appears “turned in” and the right eye “Straight” but they have actually turned in relative to each other.
Strabismus can be present all of the time (tropia), when the person is fatigued, sick, or only under testing conditions (phoria), or somewhere in between (intermittent tropia). Therefore, someone can have an eso-phoria (eyes turn towards the nose only when tired, etc.), an intermittent eso-tropia (eyes sometimes turn towards the nose on their own), or an eso-tropia (eyes always turn towards nose).
Ensure Your Child’s Comfort and Eye Health
If your child shows signs of strabismus, don’t wait to seek treatment. Contact us today to schedule a consultation and learn about effective treatment options to restore your child’s eye health and comfort.